This question is one of the most common articulated in my office and I believe represents an underappreciated component of our everyday lives that can certainly impact many facets of our health including our nervous system function. In this post, I will focus on the effects of stress on the mechanical forces impacting the peripheral nerves as these forces are what we treat during surgical intervention for occipital neuralgia or carpal tunnel syndrome, usually when multiple other treatment modalities have failed. To be sure, mechanical forces are only one way in which stress affects nerve function, but I do believe that many people, including other physicians, often don’t recognize the impact that such forces have in the pathology presenting to their offices on a fairly frequent basis. For the purposes of this discussion, I’ll use the occipital nerves (those in the back of the head and neck) as our subject, but the principles articulated apply to any peripheral nerve in the body.
Physical compression of the occipital nerves can come from several anatomic structures: muscles in the neck, scar, fascia (a tough type of connective tissue) and blood vessels, specifically branches of the occipital artery. Starting with the first of these structures, the occipital nerves all pass through or around various large and powerful muscles in the neck on their course from the spinal cord outward. When muscles contract, especially suddenly and violently (e.g., during a whiplash-type event) they constrict any structure(s) passing through them. Similarly, when people are stressed, their muscles tend to be more tense and I can recall countless occasions during which patients who were ultimately diagnosed with occipital neuralgia, told me they felt their neck muscles were “too tight”. If the muscles through which the occipital nerves are squeezing those nerves more tightly than usual, (whether suddenly and very forcefully or slightly less forcefully, but constantly), those nerves will send pain signals to the brain because of the pressure being applied to them. The covering of the muscles and one of the components of their attachment to the skull and spinal column is a tissue called fascia. As you might guess, these same occipital nerves pass from within the muscles to the subcutaneous tissues (where they provide sensation to the overlying skin) by also passing through the fascia. Hence if the fascia is too tight or the opening through the fascia has been narrowed by scar tissue, those nerves will be compressed and irritated, especially as the neck moves back and forth and those nerves try to glide smoothly, but instead end up getting kinked again and again with each individual motion. I believe that this phenomenon accounts for the fact that many of my patients report worsening symptoms as the day goes on and the amount of motion in the head and neck increases.
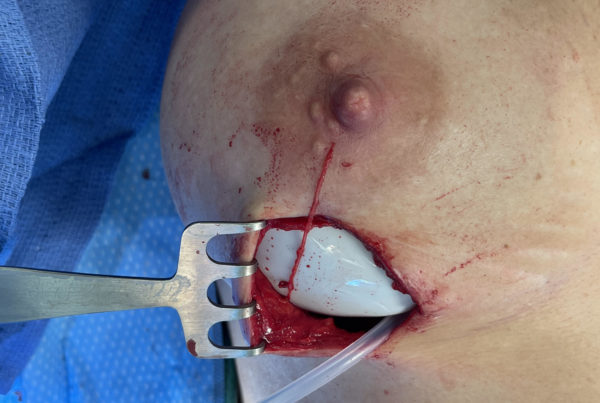
Lastly, when blood vessels are involved, the forces on the adjacent nerves take two common forms. The first is akin to that of an anaconda strangling its prey if the blood vessel is wrapped around the nerve. Alternatively, if the artery lies next to the nerve in a small and fixed space it acts like a jackhammer against pavement. In both cases, when the blood pumps through the artery with greater force, the pulsations strike the nerve with greater force. Hence, when blood pressure increases, so do the pulsatile forces on the nearby nerve, hence increasing the potential for pain. What types of things can cause blood pressure to rise? Not surprisingly, many of the same triggers that people report all the time: stress, exercise, caffeine ingestion, pain, etc. To illustrate the point, take a look at this short video of the greater occipital nerve in the process of being decompressed (LINK BELOW).
This video is a nice example of a pulsatile, occipital artery branch passing right over the greater occipital nerve which is a fairly common finding in patients suffering from occipital neuralgia. In addition, once someone experiences pain, their blood pressure rises further which in turn causes the arteries to pump harder thus causing more pain, which causes a further rise in blood pressure and setting in motion a vicious, positive feedback loop.
For all of these reasons, when we see spastic muscle, we remove small portions of the muscle to make room for the delicate nerve structures. The same is true for fascia and scar tissue. When we see vascular compression of the occipital nerves in the OR, we tie off and/or cauterize those vessels so that they no longer impact the nerves. In summary, stress can have a very real, if somewhat indirect effect on peripheral nerves as noted above and when more conservative measures (e.g., yoga, gentle stretching, meditation, biofeedback) are not enough, the focus needs to shift to the forces caused by that stress because addressing those forces is often very beneficial to the goal of pain relief.